Overview
SCART (Stereotactic Centralized Ablative Radiation Therapy) is an innovative radiation therapy technique developed by Janusyn Oncology Group for treating large, bulky, recurrent, and refractory tumors. This groundbreaking approach combines the precision of Stereotactic Body Radiation Therapy (SBRT) with the spatial fractionation concept of Spatially Fractionated Radiation Therapy (SFRT).
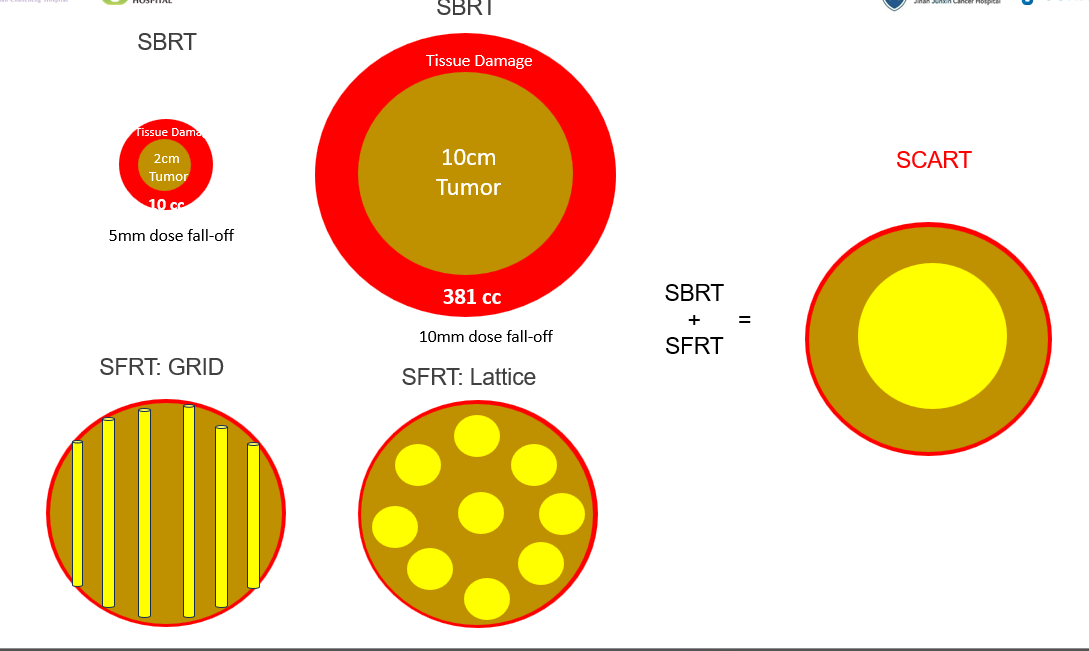
Figure 1: SCART combines SBRT and SFRT principles for treating bulky tumors
SCART Concept
SCART maximizes the stereotactic ablation of the tumor core while strictly limiting the dose to the tumor periphery. The technique leverages radiation physics dose heterogeneity coupled with intratumoral microenvironment heterogeneity to achieve optimal therapeutic outcomes.
Dose Distribution Strategy
- Ablative dose (15-24Gy x 3): Induces immunogenic tumor cell death and releases tumor-specific antigens in the "cold" tumor microenvironment at the Core
- Moderate dose (5-15Gy x 3): Drives cGAS/STING dependent I-IFN response and expression of immune susceptibility markers at the Shell
- Low dose (<3-5Gy x 3): Improves inflammatory cytokine release and immune cell trafficking and activation in "hot" TME at Periphery
- Protective dose (<3-5Gy x 3): Safe to surrounding tissue outside tumor
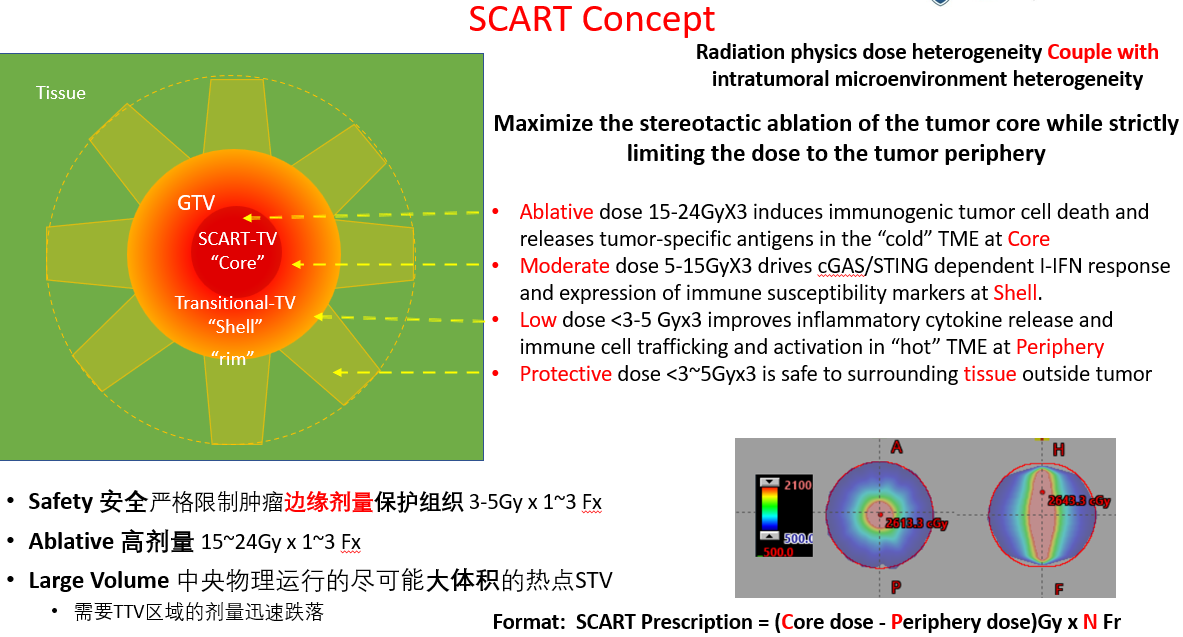
Figure 2: SCART dose distribution and immune mechanism
Comparison: CRT vs SBRT vs SCART
SCART represents a significant advancement over conventional radiation therapy techniques. While conventional radiotherapy (CRT/IMRT) provides uniform dose distribution with limited biological effectiveness, and SBRT delivers ablative doses to small targets, SCART uniquely addresses the challenge of treating large tumors by creating a controlled dose heterogeneity profile.
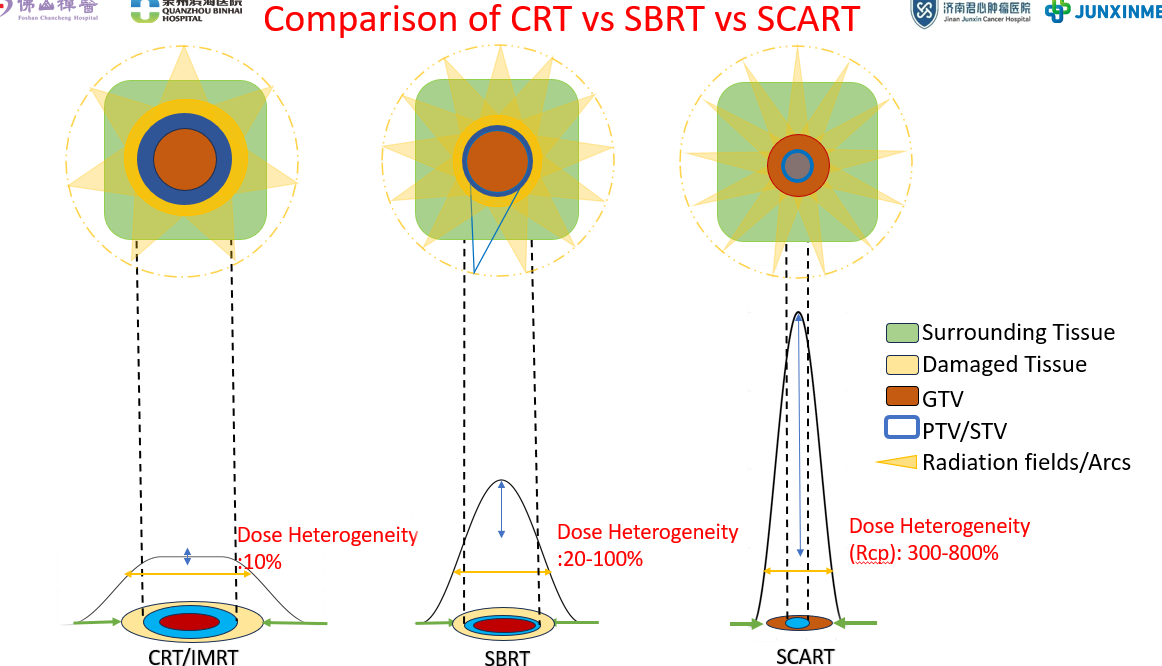
Figure 3: Dose heterogeneity comparison - CRT/IMRT (~10%), SBRT (~20-100%), SCART (300-800%)
Clinical Comparison: Grid vs Lattice vs SCART
A comparative study demonstrates SCART's superiority over existing spatially fractionated radiation techniques. The clinical comparison shows that SCART achieves significantly better target coverage while minimizing radiation exposure to surrounding healthy tissues.
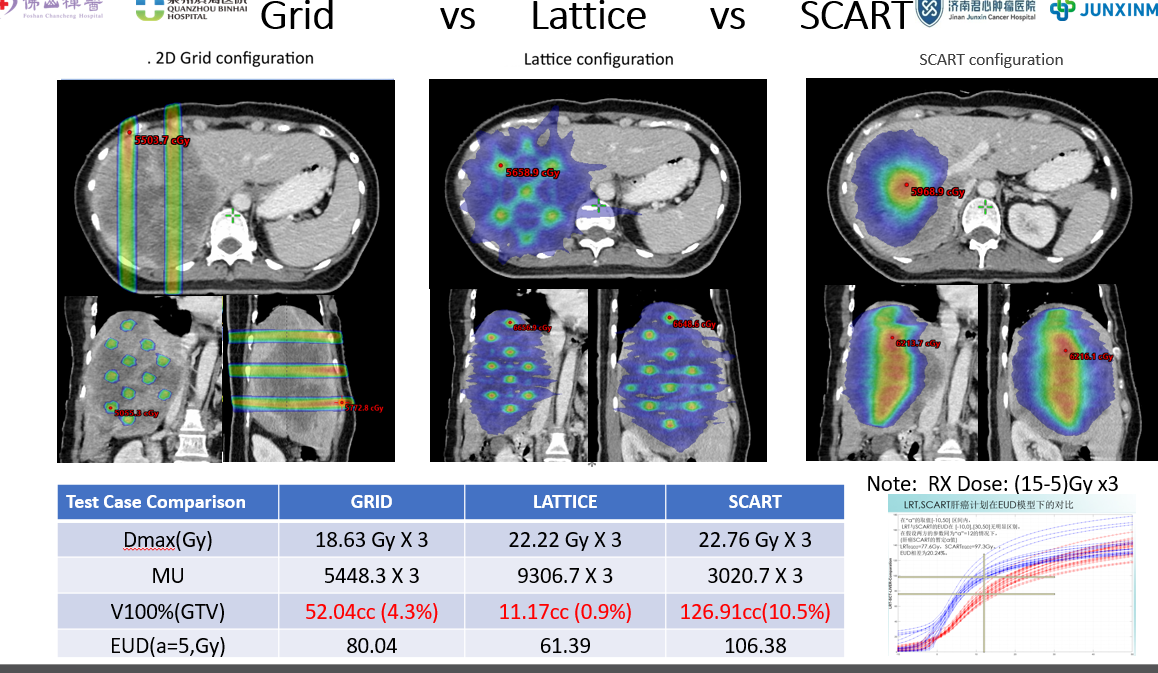
Figure 4: Clinical comparison of Grid, Lattice, and SCART configurations showing dose distribution and treatment parameters
Key Clinical Advantages
- Superior Target Coverage: SCART achieves 126.91cc (10.5%) V100% coverage of GTV compared to 52.04cc (4.3%) for GRID and 11.17cc (0.9%) for LATTICE
- Reduced Treatment Time: SCART requires only 3020.7 MU x 3 compared to 5448.3 MU x 3 for GRID and 9306.7 MU x 3 for LATTICE
- Optimal Dose Distribution: SCART provides more homogeneous dose distribution within the target while maintaining steep dose fall-off at the periphery
- Enhanced Biological Effect: Higher EUD (Equivalent Uniform Dose) of 106.38 Gy compared to 80.04 Gy for GRID and 61.39 Gy for LATTICE
Physics Behind SCART
Physics 1: Small Target = Fast Dose Fall-off
The fundamental physics principle underlying SCART is that smaller radiation fields produce faster dose fall-off at the field edge. By creating a small, high-dose central region within a larger tumor, SCART achieves steep dose gradients that protect surrounding normal tissues while delivering ablative doses to the tumor core.
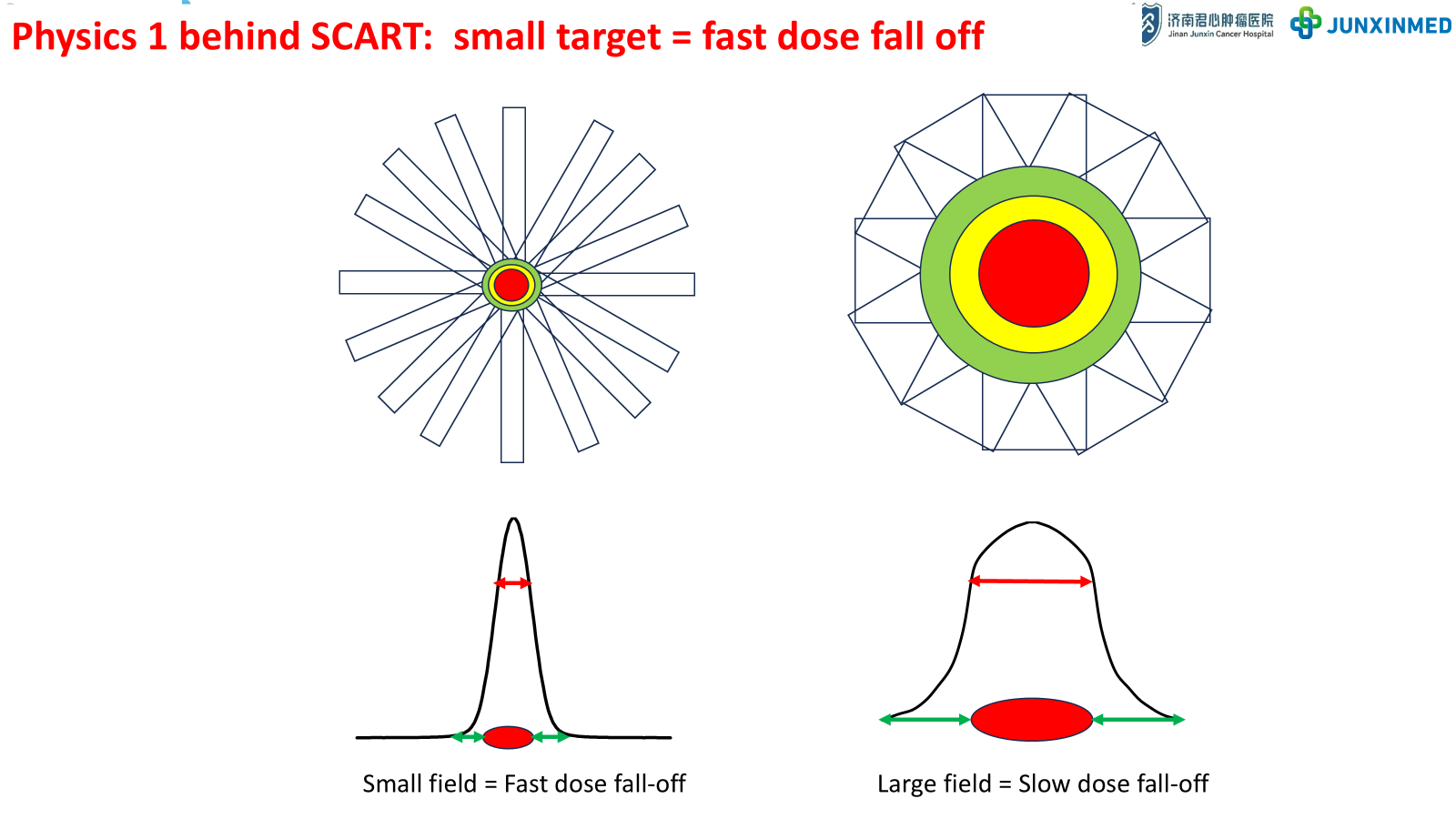
Figure 4: Small field = Fast dose fall-off
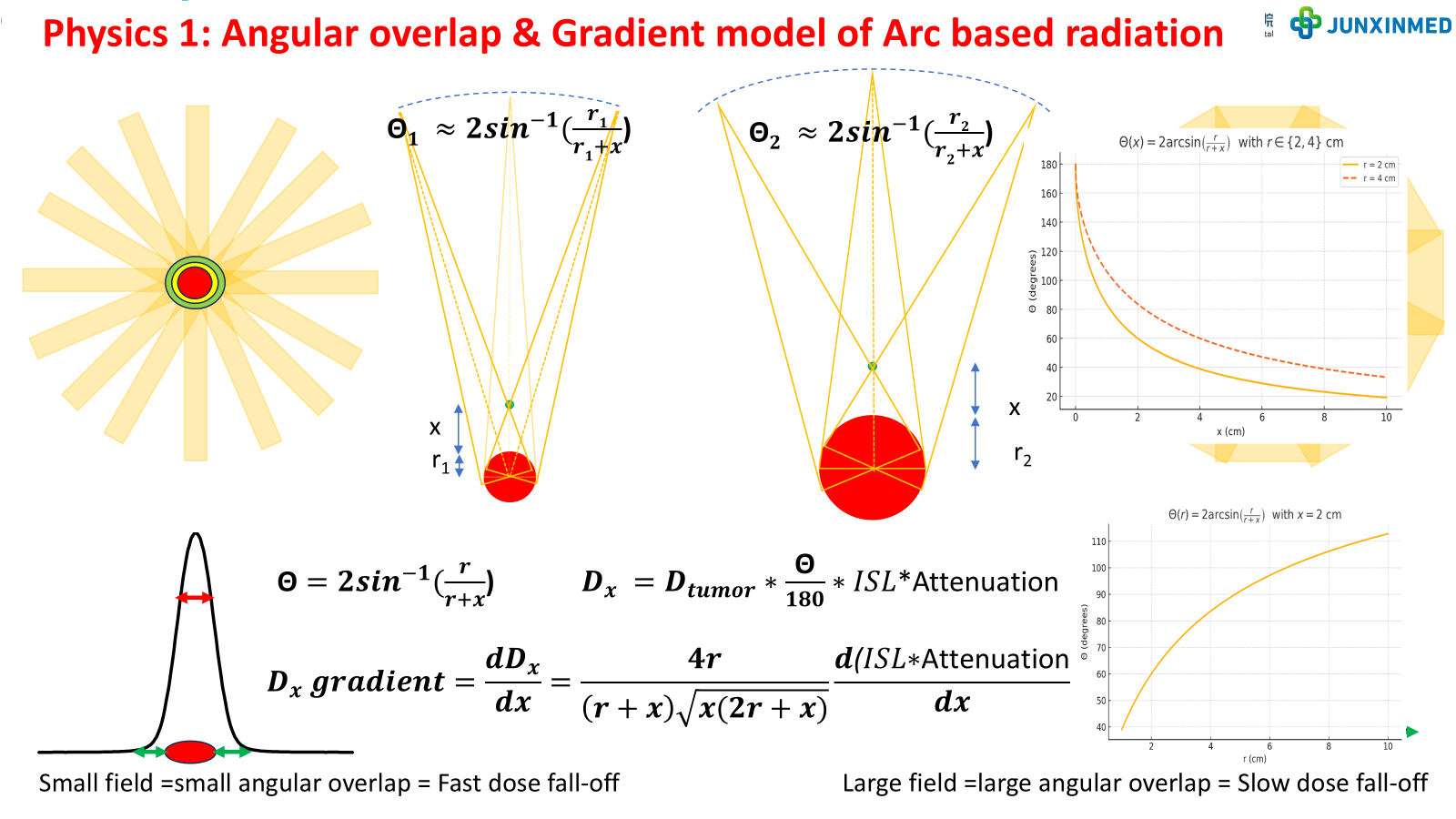
Figure 5: Angular overlap and gradient model
Physics 2: Dose Spill - At Tumor But Not Tissue
SCART strategically utilizes dose spill effects. Unlike conventional techniques where dose spill affects surrounding normal tissues, SCART confines the high-dose spill within the tumor boundaries, maximizing tumor destruction while minimizing toxicity to adjacent organs.
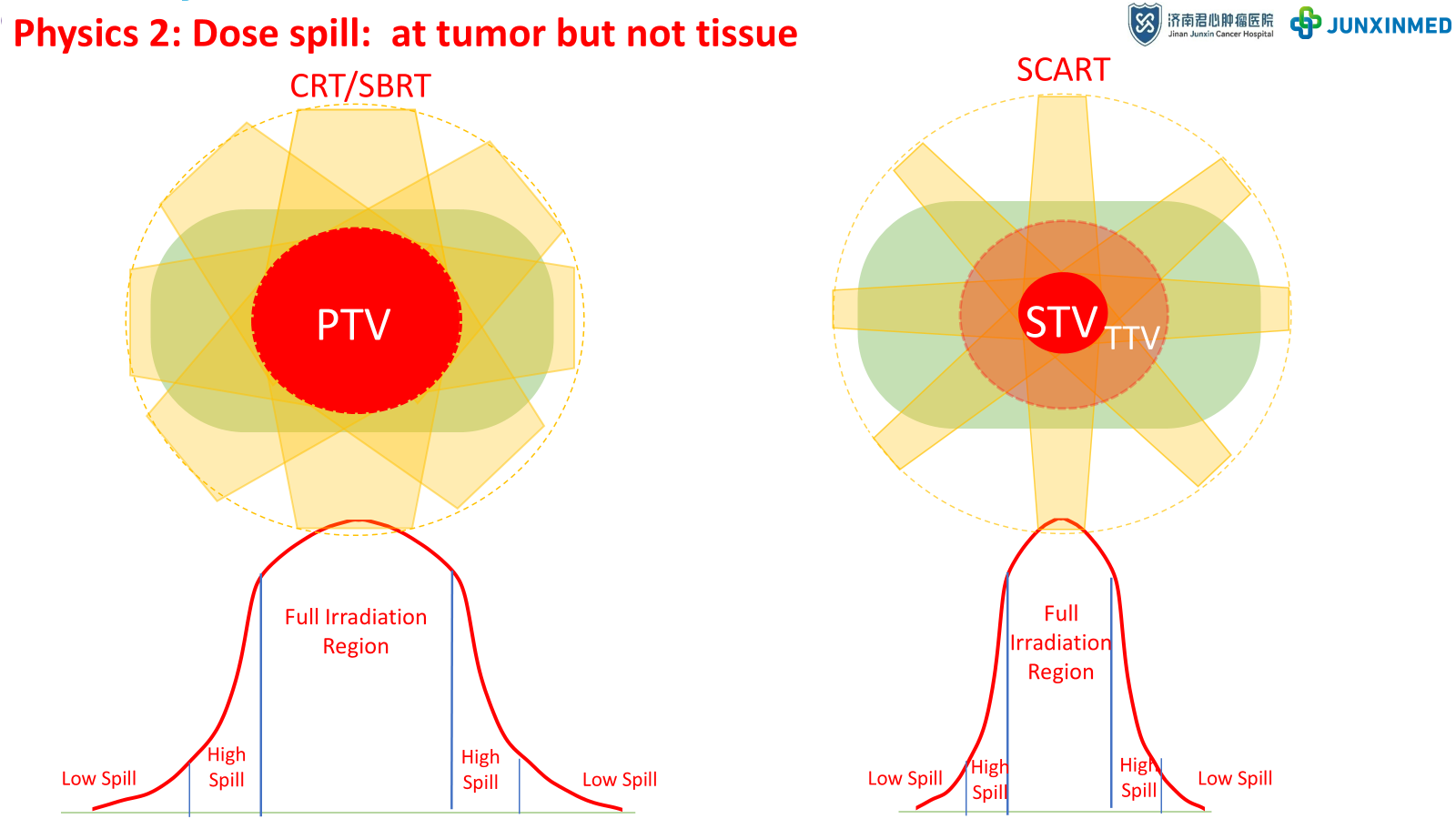
Figure 6: Dose spill comparison - CRT/SBRT vs SCART
Awards and Recognition
🏆 Best Paper Award - Radiosurgery Society 2022
In 2022, Dr. Jun Yang and the Janusyn research team received the "Best Paper of the Year" award at the Radiosurgery Society (RSS) Annual Meeting for their groundbreaking paper: "SCART Radiation Therapy Technology for Treating Large, Recurrent, and Refractory Solid Tumors". This marked the first time a Chinese research paper received this prestigious honor at the international radiosurgery conference.
Publications
📄 Frontiers in Oncology
The Janusyn Oncology Group research team's breakthrough study "Stereotactic Centralized Ablative Radiotherapy (SCART): A Phase I Study of a Novel Strategy for Treating Bulky Tumors" was published in the international peer-reviewed journal Frontiers in Oncology.
📄 IAEA ICARO-4 Presentation
Dr. Jun Yang, Chief Scientist of Janusyn Oncology Group, and Prof. Weisi Yan from University of Kentucky were invited to present at the 4th International Conference on Advances in Radiation Oncology (ICARO-4) hosted by the International Atomic Energy Agency (IAEA) in Vienna, Austria. They shared cutting-edge topics including SBRT and the pioneering SCART technology alongside leading institutions such as MD Anderson Cancer Center and Mayo Clinic.
Clinical Applications
SCART is specifically designed for challenging cases that are difficult to treat with conventional radiation therapy:
- Large/Bulky Tumors: Tumors exceeding conventional SBRT size limits
- Recurrent Tumors: Previously irradiated tumors requiring re-irradiation
- Refractory Tumors: Tumors resistant to conventional treatments
- Metastatic Disease: Large metastatic lesions requiring local control
Clinical Outcomes
Clinical studies have demonstrated promising results with SCART, showing effective local control of large tumors while maintaining acceptable toxicity profiles. The technique has been successfully applied to various tumor types including lung, liver, and metastatic lesions.
Research Team
The SCART research is led by Dr. Jun Yang, Ph.D., DABR, Chief Scientist of Janusyn Oncology Group, in collaboration with Prof. Weisi Yan, MD, PhD from University of Kentucky. The team continues to advance SCART technology through ongoing clinical trials and research collaborations.